Treatment for Health Anxiety
Treatment for Health Anxiety
Key Takeaways
Health anxiety is highly treatable, and most people improve significantly with the right support, including cognitive behavioural therapy, self-help strategies, and sometimes medication.
Your first step should be seeing a GP or primary care doctor to rule out genuine medical problems, then asking specifically about treatment options for health anxiety.
Cognitive behavioural therapy is the main evidence-based treatment, focusing on practical techniques like exposure, thought records, and reducing checking behaviours.
You can start practical self-help steps this week, such as cutting back on Googling symptoms, scheduling dedicated worry time, and gradually reducing body checking.
Seek urgent or specialist help if anxiety has lasted more than six months, causes daily distress, impacts work or relationships, or involves thoughts of self-harm.
What is health anxiety and why is treatment important?
Health anxiety is a persistent fear of having or developing a serious illness, despite medical reassurance and normal test results. You might know it by older terms like hypochondria, but the diagnostic and statistical manual now classifies it as illness anxiety disorder or somatic symptom disorder, depending on whether physical symptoms are prominent.
Living with health anxiety feels exhausting. You might find yourself repeatedly checking moles, monitoring your heartbeat, or interpreting every headache as a sign of a brain tumour. A racing heartbeat after climbing stairs becomes evidence of heart disease. A brief tingle in your arm triggers fears of multiple sclerosis. These worries consume your time worrying about your health, even when doctors confirm everything is within the normal range.
Research suggests that health anxiety affects around 1–5% of adults in any given year, with some studies finding it present in up to 10% of primary care patients. Without treatment, health anxiety typically lasts at least six months and often much longer—some untreated cases persist for five to ten years.
The impact extends far beyond worry. Health anxiety can interfere with your daily life, affecting work performance, straining relationships, disrupting sleep, and making it difficult to enjoy life. You might avoid normal activities like exercise or travel because you fear triggering symptoms. Medical bills accumulate from repeated medical tests that keep coming back normal. You seek reassurance from family, friends, or the internet, but relief never lasts.
Here’s what matters most: health anxiety is common, well-researched, and treatable. Whether you’re constantly worried about cancer, heart disease, or another specific illness, effective treatments exist. The rest of this article will focus on concrete treatment options and practical steps you can take to start overcoming health anxiety.
How is health anxiety diagnosed and when should I seek help?
The typical first step is booking an appointment with a GP or primary care physician. During this visit, you’ll discuss your symptoms in detail, and your doctor will conduct appropriate examinations to rule out any serious medical condition that might explain your concerns.
Doctors use established criteria from resources like the diagnostic and statistical manual (published by the american psychiatric association) to identify illness anxiety disorder. They may also use screening questionnaires to assess the severity of your health worries. Your doctor will want to understand how long symptoms have persisted, how much distress they cause, and how they affect your functioning.
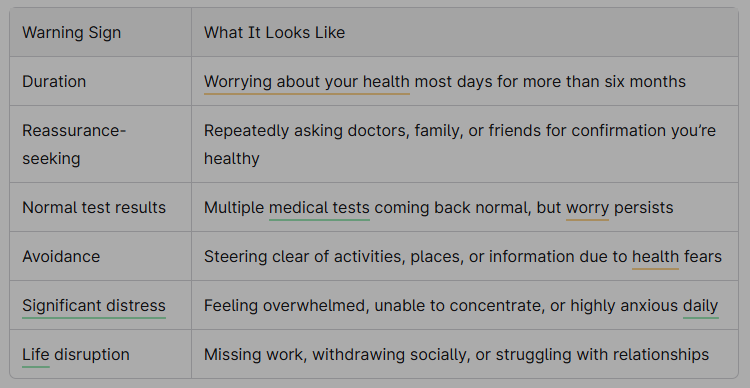
When to seek help
Consider booking an appointment if you recognise any of these patterns:
People with long-term physical illnesses—diabetes, IBS, migraines, or other conditions—can also develop health anxiety. Having a real medical condition doesn’t disqualify you from also experiencing health anxiety about new bodily feelings or disease progression. This combination is still very treatable.
If your anxiety is accompanied by persistent low mood, panic attacks, or thoughts of self-harm, seek a prompt assessment from a mental health professional. Many mental disorders co-occur, and addressing them together improves outcomes.
Evidence-based psychological treatments for health anxiety
Psychological therapies are the first-line treatment for health anxiety, supported by controlled studies dating back to the 1990s. These talking therapy approaches, especially cognitive behavioural therapy for anxiety, address the thoughts, behaviours, and emotions that keep health worries going.
Cognitive Behavioural Therapy (CBT)
Cognitive behavioural therapy is the main evidence-based approach, recommended by the national institute for Health and Care Excellence and other major guidelines, and in many areas can be accessed as free NHS CBT therapy. CBT is structured, time-limited (typically 8–20 sessions), and focuses specifically on breaking the patterns that maintain your anxiety.
Key CBT techniques for health anxiety include:
Identifying and challenging catastrophic thoughts – Learning to spot when you jump from “I have a headache” to “I must have a brain tumour” and examining the evidence for and against such conclusions
Reducing checking and reassurance-seeking – Gradually cutting back on scanning your body for signs of illness, checking moles, monitoring your pulse, and asking others if you look unwell
Limiting online symptom searching – Setting boundaries on how much time you spend researching symptoms on health websites
Graded exposure – Gradually facing feared situations like watching medical tv programmes, exercising despite bodily sensations, or reading about illness
Behavioural experiments – Testing predictions by, for example, postponing a GP visit and observing what actually happens
Research consistently shows CBT outperforms waitlist controls, with effect sizes around 1.0–1.5 on anxiety measures. Studies report that 60–70% of people show significant improvement, and gains are typically maintained at follow-up assessments.
Other evidence-based approaches
Acceptance and Commitment Therapy (ACT) takes a different angle. Rather than directly challenging anxious thoughts, ACT helps you accept uncertainty and change your relationship with worry. You learn to notice thoughts about illness without getting caught up in them, while taking action based on your values rather than your fears.
Mindfulness-based approaches complement these therapies by teaching present-moment awareness. Instead of being easily alarmed by every normal body sensations, you practise observing physical sensations without immediately labelling them as dangerous.
These therapies can be delivered in various formats:
One-to-one sessions with a therapist
Group therapy programmes
Guided self-help with therapist support
Online video sessions (telehealth)
What happens in a typical CBT programme for health anxiety?
Assessment and understanding your pattern
The first sessions focus on assessment and building a personalised picture of your health anxiety. You and your therapist will map out your “vicious cycle”—how triggers lead to catastrophic thoughts, which produce anxiety, which drives checking or avoidance behaviours, which ultimately reinforces more anxiety.
For example, you might identify that feeling a racing heartbeat (trigger) leads to thoughts like “This could be a heart attack” (catastrophic interpretation), which causes intense anxiety, which prompts you to check your pulse repeatedly and search symptoms online (safety behaviours), which temporarily reduces anxiety but keeps the cycle going.
Setting specific goals
Together, you’ll set specific, measurable goals. These might include:
Reduce daily symptom Googling from two hours to fifteen minutes by week six
Cut body checking from ten times daily to twice daily
Resume one avoided activity each week
Practical homework tasks
Most sessions include homework between appointments. You might:
Keep a thought diary when new symptoms appear, recording the symptom, your automatic thought, your anxiety level, and a more balanced alternative interpretation
Delay reassurance requests by thirty minutes and rate how your anxiety changes over time
Try feared but safe activities like gentle exercise, travelling away from home, or attending a health screening without excessive preparation
Relapse prevention
Towards the end of treatment, sessions focus on maintaining gains. You’ll learn to recognise early warning signs that health anxiety might be returning—perhaps increased Googling or more frequent medical appointments—and create a written plan for responding early.
A brief example
Consider someone who feared heart disease because of frequent palpitations. They avoided exercise entirely, checked their pulse dozens of times daily, and had visited A&E multiple times. Through CBT, they learned that palpitations are often caused by anxiety itself, not cardiac problems. They gradually reduced pulse-checking, started walking again, and tested the prediction that exercise would trigger a heart attack. After twelve sessions, they had resumed normal activities and no longer spent hours worrying about their heart.
Self-help strategies you can start using now
While you’re waiting for therapy or alongside professional help, practical self-help strategies can make a real difference. These approaches are grounded in the same principles as CBT and can help you gradually reduce health worries.
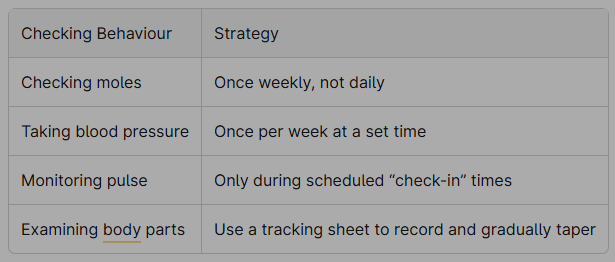
Reduce checking behaviours
Schedule worry time
Rather than letting health worries intrude throughout the day, schedule a specific “worry time”—perhaps fifteen to twenty minutes in the early evening. When worries pop up during the day, note them briefly and postpone them to your scheduled time. Many people find that by the time worry time arrives, the concerns feel less urgent.
Set rules for online searching
Online symptom searching—sometimes called cyberchondria—tends to increase rather than reduce health anxiety. Try these boundaries:
No symptom Googling after 8 p.m.
Limit searches to ten minutes maximum
Use only reputable sites (NHS, recognised medical institutions)
Notice how you feel before and after searching—if it increases anxiety, it’s not helping
Practice balanced thinking
When you notice a symptom triggering fear, write down:
The feared illness (e.g., “brain tumour”)
Evidence supporting this fear
Evidence against this fear
At least one alternative, non-catastrophic explanation (e.g., “tension headache from stress”)
This exercise helps develop different interpretations for normal body sensations rather than automatically jumping to catastrophic conclusions.
Use grounding and relaxation techniques
When anxiety spikes after noticing a new physical sensations, try:
Slow breathing – Inhale for four counts, hold for two, exhale for six
5-4-3-2-1 grounding – Name five things you can see, four you can hear, three you can touch, two you can smell, one you can taste
Progressive muscle relaxation – Systematically tense and release muscle groups
Support your body and mind
Lifestyle factors influence anxiety levels:
Regular physical activity (aim for 150 minutes weekly if your health status allows)
Consistent sleep routine (7–9 hours nightly)
Reduced caffeine and alcohol
Staying socially connected rather than isolating
These won’t cure health anxiety alone, but they create a foundation that makes other treatments more effective. Combined approaches show 50–70% remission rates compared to 30–40% for therapy alone.
Medication and combined treatments
Medication is usually considered when health anxiety is moderate to severe, when psychological therapy alone hasn’t been sufficient, or when therapy isn’t currently available. Medication decisions should always be made with a GP or psychiatrist, taking into account your medical history, current medications, potential pregnancy, and personal preferences.
Commonly prescribed medications
Doctors typically prescribe SSRIs (selective serotonin reuptake inhibitors) such as:
Fluoxetine
Sertraline
Paroxetine
Less commonly, clomipramine (a tricyclic antidepressant) may be used, based on evidence from trials on health anxiety and related anxiety disorders.
These medications work by modifying serotonin pathways in the brain, gradually reducing overall anxiety and obsessive thinking patterns. They typically take several weeks to reach full effect—often four to six weeks—so patience is required, and some people explore therapy when anxiety medication isn’t working or as a way to build longer-term coping skills alongside meds.
Effectiveness and considerations
Research shows SSRIs achieve response rates of 40–60% for health anxiety symptoms. However, medication alone is less effective than combined treatment. Studies suggest that combining CBT with medication produces better outcomes for some people than either treatment alone.
Important points to discuss with your doctor:
Expected timeline for improvement
Potential side effects (which often settle within the first few weeks)
How long to continue medication if it helps
The importance of gradual tapering rather than stopping suddenly
Stopping medication abruptly can cause discontinuation symptoms and increase relapse risk. Any changes should be planned and supervised by medical professionals.
How to find the right support for health anxiety
Finding appropriate help can feel daunting, but several routes exist depending on your location and circumstances.
NHS Talking Therapies (England)
In England, NHS Talking Therapies (formerly IAPT) provides free access to psychological therapies including CBT, and many people now self-refer to NHS mental health services rather than waiting for a GP referral. You can:
Self-refer directly without seeing your GP first
Ask your GP to refer you
Search for your local service online, and you can also draw on additional anxiety resources and recovery stories to understand what treatment and progress can look like.
When contacting services, ask specifically for help with “health anxiety” or “illness anxiety” so triage staff understand your main difficulty and can direct you appropriately.
Finding private therapists
If you’re considering private therapy, use reputable directories, or explore flexible options such as online therapy for anxiety:
British Association for Behavioural and Cognitive Psychotherapies (BABCP)
British Psychological Society (BPS)
Counselling Directory
Guides on finding the right therapist for social anxiety can also be helpful, even if your main concern is health anxiety, because many of the same principles apply when choosing a specialist.
Search for practitioners who list health anxiety, illness anxiety, or OCD-spectrum conditions as specialities, such as those offering dedicated anxiety therapy and counselling in Glasgow.
Questions to ask potential therapists
Before committing to therapy, consider asking:
What experience do you have treating health anxiety specifically?
What therapeutic approach do you use (CBT, ACT, other)?
How many sessions would you typically recommend?
Do you offer online appointments?
What are your fees and cancellation policies?
Lower-cost options
Some charities, universities, and community clinics offer therapy at reduced rates or sliding-scale fees. University training clinics, for example, provide supervised therapy from trainees at lower cost.
If therapy isn’t working
It’s acceptable to change therapist if the fit doesn’t feel right. Research consistently shows that a good therapeutic relationship is a strong predictor of progress. If you’ve given therapy a fair trial (usually at least six sessions) and don’t feel it’s helping, discuss this with your therapist or consider seeking a different provider.
Living well with uncertainty and preventing relapse
A core truth about health: no one can have 100% certainty. Even the most thorough medical care cannot guarantee perfect health forever. Learning to live with “good enough” certainty—rather than demanding absolute reassurance—is central to recovery from health anxiety.
Building tolerance for uncertainty
This involves:
Reducing the urge to double-check – Resisting the pull to verify symptoms repeatedly
Practising “maybe, maybe not” acceptance – Acknowledging uncertainty without demanding definite answers
Choosing valued activities despite worry – Living your normal life even when some anxiety is present
The goal isn’t to feel completely certain you’re healthy. It’s to feel comfortable enough with uncertainty that you can stop worrying constantly and get on with your life.
Creating a relapse prevention plan
Before finishing therapy (or as part of self-help), create a written plan that includes:
Maintaining resilience
Ongoing habits that support long-term wellbeing include:
Regular therapy check-ins if helpful (some people benefit from occasional booster sessions)
Continued use of CBT tools when needed
Maintaining a balanced routine of work, rest, and enjoyable activities
Staying connected with supportive people
Occasional spikes in health anxiety are normal, especially during stressful life events or when facing new health risks. A temporary increase doesn’t mean you’re back at square one. Using the skills you’ve learned early can prevent a brief spike from becoming a full relapse.
Frequently Asked Questions
Can health anxiety ever fully go away, or will I always have it?
Many people experience a major reduction in symptoms after targeted treatment. For some, health anxiety becomes a minor, manageable background concern rather than a dominating presence. Research shows that treated cohorts regain 70–80% of their normal functioning.
Like other anxiety disorders, health anxiety can flare up during stressful times—illness in the family, major life changes, or periods of uncertainty. However, using CBT tools early typically prevents these flares from becoming overwhelming again.
The goal of treating health anxiety isn’t to eliminate all concern about your body—some awareness of your health condition is appropriate and healthy. The aim is keeping worry at a realistic level that doesn’t control your daily life.
Is it still health anxiety if I do have a real medical condition?
Yes. People with genuine long-term conditions—asthma, heart disease, autoimmune disorders, or history of childhood illness—can also develop health anxiety about new symptoms or disease progression. Having a family history of serious illness or experiencing a health problem in early or middle adulthood can sometimes trigger excessive worry.
Treatment focuses on the excessive, persistent fear and unhelpful behaviours like constant checking and repeated unnecessary tests—not on ignoring legitimate medical advice. The approach emphasises collaboration: working with both medical professionals and mental health professionals to balance appropriate monitoring with reduced anxiety.
What if my doctor misses something serious while treating my health anxiety?
This is one of the most common and understandable fears people have when considering treatment. It’s important to know that good care includes a thorough initial medical assessment before focusing on psychological treatment.
Part of effective treatment involves agreeing with your GP on reasonable thresholds for reassessment. For example, you might agree that a new symptom lasting longer than two weeks, sudden severe pain, or specific red flags warrant review. This creates a safety net that allows you to reduce unnecessary worry while ensuring genuine concerns receive appropriate medical care.
How long does treatment for health anxiety usually take?
For CBT programmes, a typical range is 8–16 weekly sessions, though complex or long-standing cases may require longer. Most sessions last 50–60 minutes. Some people notice improvement within the first few sessions, while others see gradual change over several months.
Self-help approaches may bring noticeable change over a few weeks if used consistently. However, entrenched patterns that have persisted for years usually benefit from guided therapy rather than self help alone.
Discuss expected treatment length and specific goals with your therapist during the first couple of meetings. Having clear benchmarks helps you track progress and adjust the approach if needed.
Can I treat health anxiety on my own without seeing a therapist?
Some people do significantly improve with high-quality self help guide resources, structured online programmes, and consistent practice of CBT techniques. A good self help approach can teach you how your body works, help you develop balanced thoughts, and guide you to gradually reduce checking behaviours, including anxiety-related physical symptoms such as waking with nausea every morning.
However, anyone experiencing severe distress, thoughts of self-harm, or major life disruption should seek professional support rather than relying solely on self-help. If your health anxiety is affecting your ability to work, maintain relationships, or carry out normal activities, a mental health professional can provide the structured support needed.
Where possible, combining self-help tools with at least occasional professional input works well. A therapist can tailor strategies to your specific situation and help you navigate setbacks, increasing your chances of sustained improvement, for example through specialist anxiety therapy in Glasgow.
Recovery from health anxiety is achievable. Whether you start with self-help strategies this week, book an appointment with your GP, or self-refer to talking therapies, you’re taking a meaningful step toward reclaiming your normal life. The skills you learn in treatment stay with you—ready to use whenever health worries try to take over again.