NHS – What Is Anxiety?
Key Takeaways
Anxiety is a normal human emotion that everyone experiences, but it becomes a mental health concern when feelings are constant, overwhelming, or hard to control and start affecting your daily life.
The NHS recognises several anxiety disorders, with generalised anxiety disorder (GAD) being one of the most common long-term forms that causes persistent worry about many different aspects of everyday life.
Symptoms of anxiety include both psychological signs (constant worry, difficulty concentrating, irritability) and physical symptoms (racing heartbeat, sweating, muscle tension, stomach problems).
You should consider seeking help if you’ve been feeling anxious most days for several weeks and it’s affecting your ability to work, sleep, or maintain relationships.
Effective NHS treatments include cognitive behavioural therapy (CBT), other talking therapies, medication, and self help strategies—recovery or good symptom control is realistic for most people.
Introduction: Understanding Anxiety in the NHS Context
Feeling anxious before a job interview, an exam, or a medical appointment is perfectly normal. In fact, it’s something everyone experiences at some point. But when anxiety becomes a constant companion that won’t switch off—even when there’s no obvious reason to worry—it may be time to seek support.
This article focuses on understanding anxiety when it becomes a problem that the NHS can help with. We’ll cover what anxiety actually is, how to recognise the symptoms, what causes it, and most importantly, how and when to get NHS help, including what to do in a crisis.
The information here is aimed mainly at adults in the UK and uses NHS pathways and terminology. However, children and young people can also experience anxiety, and we’ll touch on that briefly later.
What this article covers:
A clear definition of anxiety according to the NHS
The difference between normal worry and anxiety disorders
Common symptoms of anxiety and how they affect life
When and how to seek NHS help
Treatment options including therapy and medication
Self help strategies for managing anxiety
What Is Anxiety? (NHS Definition)
Anxiety is a feeling of unease, such as worry, fear, or nervousness. It’s something everyone experiences, particularly before stressful or challenging events. You might feel anxious before sitting an exam, attending a job interview, or waiting for medical test results.
In small doses, feeling anxious can actually be helpful. It makes you more alert and focused, helping you prepare for challenges ahead. This is part of your body’s natural danger response—an evolutionary survival mechanism that kept our ancestors safe from threats.
However, anxiety becomes a problem when:
The feelings are intense and overwhelming
Worry happens frequently, even when there’s no clear danger
It continues for weeks or months without letting up
It significantly interferes with your everyday life
Anxiety involves both mind and body. Psychologically, you might experience constant worrying thoughts, a sense of dread, or fears that something terrible will happen. Physically, your body responds with changes like a racing heartbeat, faster breathing, sweating, or tense muscles. These physical symptoms happen because your brain releases stress hormones like adrenaline and cortisol as part of the fight-or-flight response.
The NHS uses the term “anxiety disorder” when anxiety is persistent, difficult to control, and significantly affects daily activities such as work, study, relationships, or self-care. There are several different types of anxiety disorders recognised by NHS services, each with their own characteristics.
What Is Generalised Anxiety Disorder (GAD)?
Generalised Anxiety Disorder (GAD) is a long-term anxiety disorder where a person feels anxious or worried most days, about a wide range of everyday things. Unlike specific phobias where there’s one clear trigger, people with GAD worry about many different issues—health, money, family, work, safety—often all at once.
With GAD, worries typically feel difficult or impossible to control. Your mind may jump from one concern to another, and the level of worry is usually more intense or persistent than what other people might experience in similar situations.
People develop GAD often describe the experience as “never being able to switch off” or finding it impossible to relax worrying, even when they’re at home, on holiday, or when things are actually going well. There’s often a background feeling of dread feeling constantly present.
GAD commonly develops in adulthood and can last for months or years without treatment. However, it’s important to know that effective help is available on the NHS.
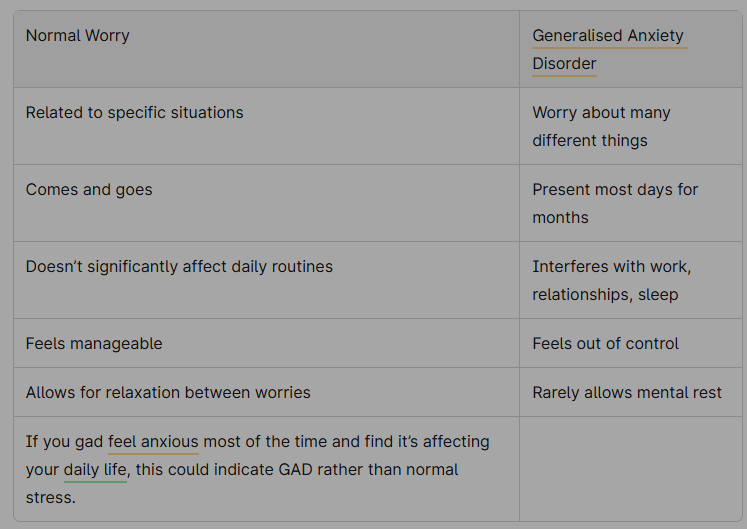
How GAD differs from normal worry:
Different Types of Anxiety Disorders Recognised by the NHS
While this article focuses on understanding anxiety generally and GAD specifically, the NHS recognises several distinct anxiety disorders. Each has its own characteristics, though the treatments often overlap.
Key anxiety disorders include:
Generalised Anxiety Disorder (GAD): Persistent, free-floating worry about many different aspects of life
Panic Disorder: Repeated panic attacks (sudden episodes of intense anxiety with overwhelming fear and physical symptoms) and ongoing fear of having more attacks
Social Anxiety Disorder: Also called social phobia, this involves intense fear of social situations and worry about being judged, embarrassed, or humiliated by others; if this sounds familiar, you may benefit from finding the right therapist for social anxiety to access effective, evidence-based treatment
Specific Phobias: Strong, disproportionate fear of particular things like heights, injections, spiders, or flying
Health Anxiety: Repeated worries about having a serious illness, often despite medical reassurance that nothing is wrong
Obsessive Compulsive Disorder (OCD): A related condition involving unwanted intrusive thoughts and anxiety compulsive behaviour, such as constantly checking things symptoms or performing rituals to reduce distress; specialist anxiety therapy and counselling can also support people living with OCD and related conditions
It’s worth noting that obsessive compulsive disorder, while related to anxiety, is sometimes classified separately. The key feature is that intrusive thoughts create anxiety compulsive behaviour patterns that the person feels driven to perform.
You may also have heard of post traumatic stress disorder (PTSD), which involves anxiety following stressful or traumatic experiences. NHS services typically describe this separately, though it shares features with other anxiety disorders.
It’s entirely possible to have more than one anxiety condition at the same time, or to experience anxiety alongside other mental health conditions like depression. NHS mental health professionals assess the overall pattern of symptoms rather than focusing on a single label.
If you recognise yourself in any of these descriptions, the best approach is to seek assessment rather than trying to self-diagnose or distinguish between similar-sounding terms on your own.
Symptoms of Anxiety and GAD
Anxiety symptoms can be grouped into three main categories: psychological (thoughts and feelings), physical (bodily sensations), and behavioural (actions and habits). For further reading, you can explore a range of anxiety resources and recovery stories that describe how others experience and manage these symptoms. Different people experience different combinations, and the main symptom for one person might be barely noticeable for another.
Psychological Symptoms
Common mental symptoms include:
Constant worry that’s difficult to control
A persistent sense of dread or that something terrible will happen
Sleep difficulty concentrating fear that affects work and daily tasks
Feeling on edge, restless, or unable to relax
Irritability and short temper
Racing thoughts that jump from one worry to another
Fear of the worst happening or losing control sweating when stressed
Intrusive thoughts about future feeling tearful or overwhelmed
Low mood that often accompanies prolonged anxiety
Physical Symptoms
The physical symptoms of anxiety can be extensive and vary from person to person. Common experiences include:
Noticeable heartbeat feeling lightheaded or dizzy
Racing heartbeat feeling faint during intense anxiety
Hot shaking mental symptoms that accompany panic
Physical symptoms faster breathing when anxious
Sweating, particularly palms and underarms
Muscle tension, backache, or other aches
Stomach churning, nausea, or lips feeling sick
Changes in appetite and toilet habits
Pins and needles in hands or feet
Dry mouth and difficulty swallowing
Headaches and feeling generally unwell
Some people experience panic attacks—sudden episodes of overwhelming fear accompanied by intense physical symptoms like chest pain, feeling unable to breathe, and a sense of losing control.
How Symptoms Affect Daily Life
Feelings of anxiety can significantly interfere with how you function. Common examples include:
Avoiding situations that might trigger worry (busy shops, public transport, social events)
Calling in sick to work when anxiety feels unmanageable, or feeling persistent anxiety before work every morning
Leisure time difficulty—being unable to enjoy hobbies or relaxation
Struggling to maintain relationships worried about burdening others
Difficulty making decisions, even small ones
Repeatedly seeking reassurance from family members
Changes in sleep patterns—either sleeping too much or insomnia
Reduced sex drive and physical intimacy
Important note: Anxiety can sometimes be mistaken for physical health problems. Chest pain might be mistaken for a heart problem, or digestive issues for a stomach condition. NHS clinicians will usually check for physical causes before confirming anxiety as the main issue. This is why being honest about all your symptoms is so important.
Anxiety Triggers: When There Is and Isn’t a Clear Cause
Understanding what triggers anxiety can be helpful for managing it, though identifying triggers isn’t always straightforward.
Clear Triggers
In some anxiety disorders, anxiety triggers are obvious and specific:
Specific phobias: Confined spaces, injections, flying, heights, certain animals
Social anxiety: Public speaking, meeting new people, being watched while eating
Panic disorder: Sometimes triggered by specific situations, though often panic attacks seem to come from nowhere
GAD and Unclear Triggers
With generalised anxiety disorder, the anxiety often doesn’t have one obvious trigger. It may appear to “come out of the blue” or shift quickly from one worrying topic to another. You might wake up feeling anxious without knowing why, or find that anxiety symptoms worsen without an obvious cause.
Common everyday triggers that can increase GAD symptoms:
Reading worrying news stories or scrolling social media
Work emails arriving late at night
Family conflict or relationship tension
Letters about finances, bills, or official matters
Health-related searches online (which often make health anxiety worse)
Major life changes, even positive ones like moving house
Uncertainty about the future
When Not Knowing Becomes the Problem
For many people, the uncertainty itself becomes a source of anxiety. Not knowing why you feel physically unwell or anxious can create additional worry. Some people become anxious about “feeling anxious,” fearing they’re losing control or that symptoms will never stop.
Practical tip: Keeping a simple diary of situations, thoughts, and bodily feelings can help identify patterns that aren’t obvious in the present moment. Note what was happening before anxiety increased, what thoughts went through your mind, and what physical symptoms you noticed. This information can be valuable to share with a GP or therapist.
What Causes Anxiety and GAD?
There is rarely a single exact cause of anxiety. Instead, anxiety disorders typically arise from a combination of biological, psychological, and social factors.
Biological Factors
Family history: Having a close family member with anxiety or depression increases risk
Brain chemicals serotonin and other neurotransmitters: Differences in how the brain involved in mood regulation functions may contribute
Physical health conditions: Some conditions like thyroid problems can mimic or worsen anxiety
Blood pressure and heart conditions: Can cause symptoms that feel like anxiety
Life Experiences
Certain life experiences significantly increase the risk of developing an anxiety disorder:
Long-term stress at work or home
Bereavement or loss
Relationship breakdown
Serious illness in yourself or a family member
Financial difficulties and money worries
Traumatic experiences including domestic violence child abuse or other abuse
Drug or alcohol misuse, which can both cause and worsen anxiety
Major life transitions
Stressful or traumatic experiences, particularly in childhood, can shape how your brain responds to stress throughout life. Domestic violence, child abuse, neglect, or other forms of trauma are significant risk factors for developing anxiety disorders later.
Personality and Thinking Patterns
Some people may be more prone to anxiety due to:
A tendency to imagine worst-case scenarios
Perfectionism and high standards
Feeling responsible for preventing bad things from happening
Difficulty tolerating uncertainty
Low self-esteem
Who Is Most Affected?
Research and NHS data suggest:
Anxiety disorders are more commonly reported by women than men
GAD often emerges in early to mid-adulthood
Anyone can be affected regardless of background
However, it’s crucial to remember that anxiety can affect anyone, and seeking help is always appropriate if you’re struggling.
When to Get Help for Anxiety
Knowing when to seek help can be difficult. Many people wonder if their anxiety is “bad enough” to warrant professional support, or worry about wasting NHS time.
Signs You Should Seek Help
Consider speaking to a GP if:
You’ve been feeling anxious most days for several weeks
Anxiety is affecting your daily life—work, relationships, sleep, or enjoyment of activities
Others have noticed you seem constantly worried or withdrawn
You’re avoiding situations, places, or people because of anxiety
Physical symptoms are causing significant distress
You’re using alcohol misuse or drugs to cope with stress
NHS Guidance on GAD
Typical NHS guidance suggests GAD is likely when:
Excessive, hard-to-control worry has been present on most days
Symptoms have lasted for at least six months
The worry causes significant distress or impairment
However, you don’t need to wait six months if you’re struggling. Early intervention often leads to better outcomes.
Warning Signs That Suggest Help Is Needed Now
Frequent absences from work or education due to anxiety
Avoiding leaving the house
Arguments at home linked to irritability
Using alcohol, drugs, or gambling to try to cope
Neglecting self-care (eating, washing, sleeping)
Relationships are suffering
Thoughts of self-harm
Practical Steps to Get Help
Book a GP appointment: You can describe your symptoms and how they’re affecting your daily life
Use NHS 111: If you’re unsure what to do or need advice outside GP hours
Self-refer to NHS talking therapies: In England, you can self refer to NHS mental health services directly to psychological therapy services for anxiety and depression without seeing a GP first, and many people are able to access free CBT therapy through NHS talking therapies
Speak to a health visitor: If you’re a new parent experiencing anxiety
Contact support groups: Many support groups and local support groups offer peer support
Crisis Situations
If you’re experiencing a mental health crisis, get help immediately:
Thoughts of self-harm or suicide: Contact 999, go to A&E, or call NHS 111
Unable to cope with daily life at all: Seek urgent GP appointment or NHS 111
Feeling at immediate risk: Call emergency services
You can also contact support groups and crisis helplines run by mental health charities for immediate support.
How the NHS Diagnoses Generalised Anxiety Disorder
Understanding what to expect at a GP appointment can make seeking help feel less daunting.
What Happens at a GP Appointment
Your GP will typically:
Ask about your current worries and how long they’ve been going on
Discuss how anxiety is affecting your daily life in terms of work, sleep, appetite, and relationships
Ask about both psychological and physical symptoms
Enquire about your lifestyle, including alcohol and caffeine intake
Ask about any previous treatment or support you’ve received
Check whether you’re experiencing symptoms of depression or other mental health conditions
Physical Checks
Because some physical conditions can cause anxiety-like symptoms, your GP may:
Perform a brief physical examination
Check your blood pressure and heart rate
Order blood tests to rule out thyroid problems or other conditions
Ask about any medications you’re taking
Assessment Tools
NHS clinicians often use structured questions or questionnaires to:
Assess the severity of your anxiety
Track progress over time
Determine the most appropriate level of support
Diagnostic Criteria for GAD
A diagnosis of GAD typically involves:
Excessive worry present most days
Symptoms lasting several months (often six months or more)
Difficulty controlling the worry
At least several related symptoms such as:
Restlessness or feeling on edge
Fatigue
Irritability
Muscle tension
Sleep disturbance
Difficulty concentrating
Being Honest Helps
Being honest about alcohol misuse or drug use, mood changes, and any thoughts of harm will help NHS staff recommend the safest and most effective treatment plan. Mental health specialist staff are trained to discuss sensitive topics without judgement.
Treatment for Anxiety and GAD in the NHS
The good news is that anxiety disorders, including GAD, are treatable. Many people experience significant improvement with the right support, though progress may take time.
The Stepped Care Approach
NHS treatment often follows a “stepped care” model:
Step 1: Information, self help resources, and watchful waiting
Step 2: Guided self-help, psychoeducational groups, or computerised CBT
Step 3: Individual psychological therapy (like CBT) or medication
Step 4: Specialist mental health services for complex or severe cases
This approach ensures people receive the least intensive effective treatment first, with more intensive options available if needed.
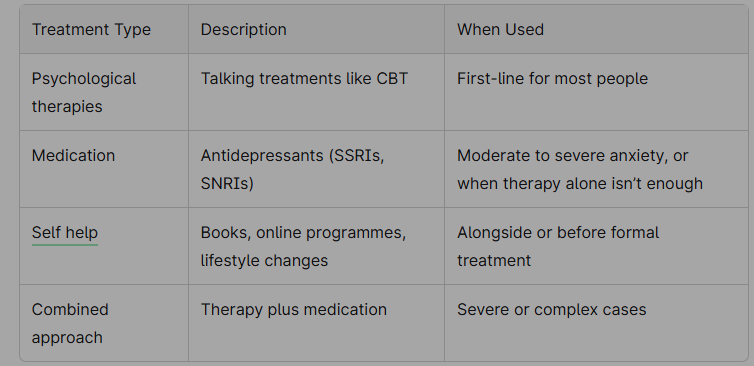
Main Treatment Options
Referral Pathways
Most people start with their GP
Direct self-referral to NHS talking therapies is available in England
Some people may be referred to a community mental health team or mental health specialist for more complex needs
Psychological Therapies for Anxiety
Talking therapies are usually the first-line treatment for anxiety disorders. They address the underlying patterns of thinking and behaviour that keep anxiety going.
Cognitive Behavioural Therapy (CBT)
Cognitive behavioural therapy cbt is considered the most effective psychological treatment for GAD. Research shows it often provides longer-lasting benefits compared to medication alone, and many services offer structured CBT for anxiety using evidence-based techniques such as gradual exposure.
How CBT works:
Based on the principle that thoughts, feelings, and behaviours are connected
Helps you identify unhelpful thinking patterns (like catastrophising)
Teaches practical skills to challenge anxious thoughts
Involves gradually facing situations you’ve been avoiding
Uses problem solving techniques for real-life challenges
Includes homework tasks between sessions
Typical CBT structure:
Weekly sessions of about one hour
Usually lasts 3-4 months (12-16 sessions)
Covers the anxiety cycle and how to break it
Focuses on your specific worries and situations
Applied Relaxation
Another evidence-based treatment that teaches you to:
Recognise early signs of tension in your body
Use specific relaxation techniques to reduce physical anxiety
Apply these skills in real-life situations before anxiety escalates
This is also delivered in weekly sessions and can be particularly helpful if physical symptoms are prominent.
Guided Self Help
A lighter form of CBT that may include:
Self help workbooks with therapeutic content
Online programmes or apps
Brief support from a therapist (by phone or in person)
Completed at your own pace
This is often recommended as an early step in NHS care and is effective for many people with mild to moderate anxiety.
Group Therapy
Some NHS services offer:
Group courses where several people learn skills together
Psychoeducational groups that explain how anxiety works
Peer support alongside professional guidance
Some people find group settings motivating and less isolating than individual therapy.
Medication for Anxiety and GAD
GPs may discuss medication when anxiety is moderate to severe, has lasted a long time, or hasn’t improved enough with psychological therapies and self help alone. If you feel your anxiety medication is not working, it can help to review options with a professional and consider therapy-focused approaches.
SSRIs (First-Line Medication)
Selective serotonin reuptake inhibitors are usually the first medication considered for GAD:
Work by affecting brain chemicals serotonin levels
Common examples include sertraline and escitalopram
Take several weeks to show full effect
Generally well-tolerated, though side effects can occur initially
Should not be stopped suddenly
SNRIs (Second-Line Option)
Serotonin and noradrenaline reuptake inhibitors like venlafaxine may be offered if:
SSRIs haven’t been effective
Side effects from SSRIs are problematic
Other Medications
Pregabalin: Sometimes considered for GAD in adults
Benzodiazepines: May be prescribed only short-term for very severe anxiety or crisis situations due to dependence risk
Important Considerations
Before starting, changing, or stopping any medication, discuss:
Potential side effects (nausea, sleep changes, initially increased anxiety)
Pregnancy and breastfeeding implications
Interactions with other medications
How long you might need to take the medication
How to reduce the dose gradually when stopping
Never stop anxiety medication suddenly without medical advice, as this can cause withdrawal symptoms.
Self-Help Strategies for Managing Anxiety
Managing anxiety effectively often involves daily practices and lifestyle changes alongside any formal treatment.
Evidence-Based Self Help Resources
NHS staff may recommend:
CBT-based books or workbooks
Online programmes (some are NHS-approved)
Apps designed for anxiety management
The key is to use these systematically rather than dipping in and out occasionally.
Relaxation Techniques
Regular practice is more effective than occasional use:
Breathing exercises: Slow, diaphragmatic breathing to calm the nervous system
Progressive muscle relaxation: Tensing and releasing muscle groups systematically
Mindfulness: Focusing attention on the present moment rather than worries
Yoga or gentle stretching: Combines physical movement with relaxation
Lifestyle Strategies
Connecting with Others
Contact support groups or local support groups for people with anxiety
Share experiences with trusted friends or a family member
Consider peer support communities (online or in person), as well as online therapy options if attending in-person sessions is difficult
Don’t isolate yourself—connection reduces anxiety over time
Many support groups offer understanding from people who’ve experienced similar challenges and can provide practical coping ideas.
Talking to Your GP or Health Professional About Anxiety
Being prepared for your appointment can help you make the most of your time with a health professional.
Preparation Tips
Before your appointment:
Keep a brief note of symptoms, triggers, and how anxiety affects your daily life
Write down how long symptoms have been present
List any medications or supplements you’re taking
Prepare questions you want to ask
Key Points to Mention
During the appointment, try to describe anxiety as clearly as you can:
How long you’ve been experiencing symptoms
What makes anxiety better or worse
Impact on work, study, relationships, and social life
Any previous treatment or support you’ve tried
Other symptoms like low mood or panic attacks
Being Open About Sensitive Topics
It’s important to mention:
Alcohol, drug, or substance use
Thoughts of self-harm or suicide
Any traumatic experiences that might be relevant
NHS staff are trained to discuss mental wellbeing and mental health without judgement. Being honest helps them provide the safest and most appropriate care.
Questions to Ask
What treatment options are available?
Can I self-refer to NHS talking therapies?
Are there digital or online options?
What are current waiting times?
What can I do in the meantime while waiting for treatment?
When should I come back for a follow-up?
Follow-Up
Follow-up appointments are often needed to review progress
If medication is started, regular check-ins help manage side effects
You can bring a trusted friend or family member if that helps
Help, Support, and Useful Organisations
Multiple sources of support are available for people experiencing anxiety.
NHS Services
GPs and practice nurses: Initial assessment, advice, and referrals
NHS talking therapies: Psychological therapy services (self-referral available in England), including access to free CBT therapy in many areas
Community mental health team: For more complex or severe cases
NHS 111: Advice when you’re unsure what to do, alongside online information on how to self refer to mental health services if appropriate
Mental Health Charities
National mental health charities offer:
Information about anxiety and other mental health conditions
Telephone helplines and online chat support
Signposting to local services
Online forums and peer support communities
Support Groups
Many areas have online or in-person support groups and anxiety resources for anxiety
Local support groups allow people to share experiences and coping strategies
Many support groups are free and open to anyone
Support for Carers and Family
If you’re supporting someone with anxiety:
You can seek advice about how to help
Carers’ organisations offer information and support
Understanding what your family member is experiencing can help you provide better support
Finding Reliable Information
Use reputable NHS or charity websites rather than unverified social media sources. Accurate information about mental wellbeing can reduce worry and help you make informed decisions.
Children and Young People: Anxiety Overview
Anxiety is also common in children and teenagers. Some worries are a normal part of development—separation anxiety in young children or exam stress in adolescents, for example.
Signs Anxiety May Be a Problem
Watch for:
Frequent stomach aches or headaches without clear physical cause
Refusing to go to school or nursery
Sleep problems—difficulty falling asleep or frequent nightmares
Clinginess or difficulty being away from parents
Sudden changes in behaviour or mood
Avoiding activities they previously enjoyed
Tearfulness or irritability
What Parents and Carers Can Do
Talk calmly with your child about their worries
Listen without dismissing their concerns
Reassure them while encouraging small brave steps
Inform school staff—class teacher, school nurse, or counsellor
When to Seek Professional Help
Contact a GP if:
Your child’s anxiety lasts for several weeks
It’s interfering with school, friendships, or family life
Your child seems very distressed
They talk about not wanting to be alive or harming themselves
A health visitor can also provide guidance for younger children.
Specialist Services
NHS children and young people’s mental health services (often called CAMHS) can offer:
Age-appropriate assessment
Family-based therapy
Individual therapy for older children
Support for parents
Living with Anxiety: What Keeps It Going and How to Break the Cycle
Understanding what maintains anxiety can help you take steps to reduce it.
The Anxiety Cycle
Anxiety typically follows a pattern:
Trigger or thought: Something happens or a worry enters your mind
Physical response: Body releases stress hormones, causing physical symptoms
Fearful interpretation: You interpret the symptoms as dangerous or that you’re losing control
Avoidance or safety behaviour: You avoid the situation or do something to feel safer
Short-term relief, long-term problem: Avoidance feels good momentarily but reinforces the anxiety
Behaviours That Keep Anxiety Going
Avoidance: Not going to places or situations that make you anxious
Reassurance-seeking: Repeatedly asking others for confirmation that things are okay
Checking: Constantly checking things symptoms won’t happen or that you haven’t made mistakes
Safety behaviours: Things you do to prevent feared outcomes (carrying medication “just in case,” always sitting near exits)
Breaking the Cycle
Gradual exposure: Instead of avoiding feared situations, approach them in small, manageable steps. Stay in the situation until anxiety naturally decreases.
Reducing reassurance-seeking: Practice tolerating uncertainty rather than seeking constant confirmation.
Dropping safety behaviours: Gradually let go of rituals or precautions that maintain anxiety.
Challenging thoughts: Question whether your predictions are realistic or helpful.
Expect Gradual Progress
Change happens through small, repeated steps
Setbacks are normal and can be learned from
Progress isn’t linear—there will be good days and harder days
Celebrate small gains, like a first short bus journey or a social visit
Each time you face anxiety rather than avoiding it, you build evidence that you can cope—and the anxiety gradually loses its power.
FAQ
Is anxiety a mental illness or just stress?
Short-term anxiety in response to life events is a normal reaction to stress. However, an anxiety disorder is considered a mental health condition when symptoms are frequent, long-lasting, and significantly interfere with daily life. NHS staff view anxiety disorders as common, treatable health problems rather than personal weakness or “just stress.” If you’re unsure whether your symptoms are normal stress or an anxiety disorder, speaking to a GP can help clarify this.
Can anxiety go away on its own without treatment?
Mild anxiety may improve when stressful circumstances change. However, long-term or severe anxiety (such as GAD) often persists or returns without some form of support or active self help. Research suggests that seeking help earlier tends to lead to better outcomes and may prevent anxiety from becoming more entrenched or leading to depression and other problems. If anxiety is already affecting your sleep, work, or relationships, it’s worth seeking support rather than waiting for it to disappear on its own.
Can physical health problems cause or worsen anxiety?
Yes, certain physical conditions can cause symptoms that feel like anxiety or make existing anxiety worse. Examples include thyroid disorders, heart rhythm problems, low blood sugar, and chronic pain conditions. This is why GPs may check blood tests, heart rate, or other physical signs before confirming a diagnosis of an anxiety disorder. Always mention all physical symptoms and medical conditions to your doctor so both physical and mental health needs can be addressed together.
Will I have to take anxiety medication forever?
Many people take anxiety medicines for a limited period—often several months to a year—while learning and practising other coping skills through therapy and self help. Decisions about starting, continuing, or stopping medication are individual and should be made together with a GP or psychiatrist, based on benefits, side effects, and personal preference. It’s important never to stop medication suddenly without medical advice, as doses usually need to be reduced gradually to avoid withdrawal symptoms.
Can I still work or study if I have an anxiety disorder?
Many people with anxiety disorders continue to work or study successfully, sometimes with adjustments such as flexible hours, quiet workspaces, regular breaks, or exam accommodations. In the UK, workplaces and educational institutions often have policies and support services for mental health. You may have legal rights to reasonable adjustments under equality legislation. Consider discussing options with managers, tutors, human resources, occupational health, or student support teams if anxiety is affecting your daily life at work or in education.