How to Handle Anxiety
Anxiety is something most people experience at some point, and the good news is that it responds well to treatment. Whether you’re dealing with occasional worry or more persistent anxious feelings, this guide will walk you through clear, practical steps to feel calmer starting today.
Key Takeaways
Anxiety is a normal human response that becomes a problem when it’s too frequent, intense, or long-lasting—affecting around 1 in 6 people in the UK, including cities like Glasgow.
Understanding your symptoms, recognising your triggers, and using simple tools like breathing exercises and grounding techniques is the fastest way to reduce anxiety in the moment.
Many people in busy urban environments mistake anxiety for physical illness; noticing patterns early and seeking support can prevent symptoms from becoming chronic.
Lifestyle changes, self-help techniques, and professional therapy work best when combined rather than used in isolation.
Start today with these three actions: practise one breathing exercise (like 4-4-8 breathing), try one grounding exercise (the 5-4-3-2-1 senses technique), and take one small behavioural step (like going somewhere you’ve been avoiding for just two minutes).
What Is Anxiety and When Does It Become a Problem?
Think of anxiety as your body’s built-in alarm system. It exists to protect you from danger by preparing you to fight, flee, or freeze. This response served our ancestors well when facing predators, and it still helps us today when we need to perform under pressure or respond quickly to genuine threats.
The problem arises when this alarm system becomes too sensitive—going off for burnt toast as well as real fires. When anxiety shows up too frequently, feels too intense for the situation, or lasts long after the trigger has passed, it stops being helpful and starts interfering with your life.
Consider some everyday examples where anxiety makes sense: feeling nervous before an exam, a driving test, a job interview in Glasgow city centre, or waiting for medical results. These situations carry genuine stakes, and some anxiety sharpens your focus. But when that same level of dread appears while reading emails, walking to the shops, or trying to fall asleep with no clear cause, something different is happening.
The key difference between normal, situational anxiety and anxiety that needs attention lies in impact. If anxiety regularly disrupts your sleep, affects your work performance, strains your relationships, or causes you to avoid situations you used to handle, it’s worth taking seriously.
Anxiety disorders—including generalised anxiety disorder (GAD), social anxiety, panic disorder, and specific phobias—are diagnosable conditions, not character flaws or signs of weakness. Research shows that around 18% of adults experience an anxiety disorder in any given year, and in the UK, roughly 1 in 6 people face mental health issues annually.
Why early recognition matters:
Anxiety symptoms that persist untreated for months or years often become harder to shift
Early intervention can prevent the development of related conditions like depression (which has a 40% co-occurrence risk with untreated anxiety)
Learning coping skills when symptoms are mild makes them easier to apply during more intense anxiety
Common Symptoms of Anxiety
Anxiety doesn’t just live in your head. It shows up in your body, your thoughts, and your behaviour—and many people initially assume they’re dealing with a physical health condition rather than anxiety. Understanding how anxiety manifests across these three areas helps you recognise what you’re experiencing.
Physical symptoms often include a racing heartbeat, tight chest or difficulty breathing, dizziness, stomach upset or nausea, sweating, trembling, muscle tension, and fatigue. Your body releases stress hormones like adrenaline and cortisol, which create these sensations as part of the fight-or-flight response.
Mental symptoms centre on persistent worry, a sense of dread, difficulty concentrating, intrusive “what if” thoughts, and feeling like something terrible is about to happen. People with anxiety often describe their mind as feeling like it won’t switch off.
Behavioural symptoms include avoidance (steering clear of situations that trigger anxiety), checking behaviours (repeatedly making sure doors are locked or emails were sent correctly), and reassurance seeking (asking others repeatedly if everything is okay).
Concrete examples help illustrate these patterns: someone might avoid Sauchiehall Street because of crowds, or they might check work emails repeatedly until midnight despite having responded to everything. Another person might decline social gatherings because the thought of small talk feels overwhelming.
Symptoms can build gradually over months—a slow creep of feeling on edge most days without obvious triggers—or they can appear suddenly after a stressful life event. Some people experience intense anxiety in specific situations while feeling fine otherwise; others feel a low-level hum of worry throughout their entire daily life.
Consider tracking your symptoms for one to two weeks using a simple notebook or phone notes. Write down when anxiety appears, what was happening at the time, how intense it felt (on a scale of 1-10), and what thoughts were running through your mind. This information becomes valuable if you decide to speak with a GP, therapist, or explore anxiety resources and recovery stories in Glasgow..
What a Panic Attack Feels Like
A panic attack is a sudden surge of intense anxiety that comes with overwhelming physical sensations. Your heart pounds so hard you might worry it’s going to burst out of your chest. You may struggle to catch your breath, feel like you’re choking, experience trembling throughout your body, and notice a strange sense of unreality—as if you’re watching yourself from outside your body or the world around you isn’t quite real.
Panic attacks typically peak within 5 to 10 minutes and usually settle within about 5 to 30 minutes, even though they can feel much longer when you’re in the middle of one. The intensity of the physical symptoms—the increased heart rate, chest tightness linked to anxiety rather than your heart, dizziness—leads many people to fear they’re having a heart attack, losing their mind, or about to die..
Here’s what’s important to understand: medically assessed panic attacks are not dangerous or life-threatening. The sensations are deeply unpleasant and frightening, but they cannot harm you. Your body is simply experiencing an extreme version of its normal stress response.
That said, if you experience chest pain for the first time, have symptoms that are new or different from previous panic attacks, or feel genuinely uncertain about what’s happening, seek urgent medical advice. It’s always worth ruling out physical causes the first time these symptoms appear.
One challenge with panic attacks is that they can create a fear of having another one. This anticipatory anxiety might lead you to avoid situations where attacks have happened before—buses, trains, crowded shops, or specific places like the Glasgow subway at rush hour. This avoidance can gradually shrink your world, which is why learning to handle panic attacks is so valuable.
What’s Happening in Your Body When You Feel Anxious?
When you feel anxious, your brain’s alarm centre—the amygdala—has detected what it perceives as a threat. It doesn’t distinguish well between a genuine emergency and a worrying thought, so it triggers the same response either way.
This triggers your sympathetic nervous system to release stress hormones, primarily adrenaline and cortisol. These chemicals prepare your body for action: your heart rate increases to pump blood faster to your muscles, your breathing quickens to take in more oxygen, your muscles tense ready to move, and your senses sharpen. Digestion slows down (not a priority when you’re supposedly running from danger), which explains the stomach upset many people experience with anxiety.
Consider the triggers that might set this off in daily life: your phone rings from an unknown number. You’re packed into a crowded Glasgow subway carriage at rush hour with strangers pressing against you. You hear rumours about layoffs at work. Your brain interprets each of these as potential threats and fires up the same ancient protection system.
The reassuring news is that these body changes are entirely reversible. Your parasympathetic nervous system—the “rest and digest” response—can bring everything back to baseline. With practice and support, you can train your nervous system to calm down more quickly after anxiety spikes.
Think of it like a smoke alarm that’s become oversensitive. The alarm going off doesn’t mean there’s actually a fire—sometimes it’s just burnt toast. Your job isn’t to disconnect the alarm entirely (you need it for real emergencies), but to recalibrate it so it responds proportionately.
Identify Your Anxiety Triggers and Patterns
Not all anxiety has an obvious cause. Sometimes it seems to appear from nowhere, a free-floating sense of dread that attaches to whatever crosses your mind. However, many people do have identifiable triggers, and recognising these patterns gives you more control and choice in how you respond.
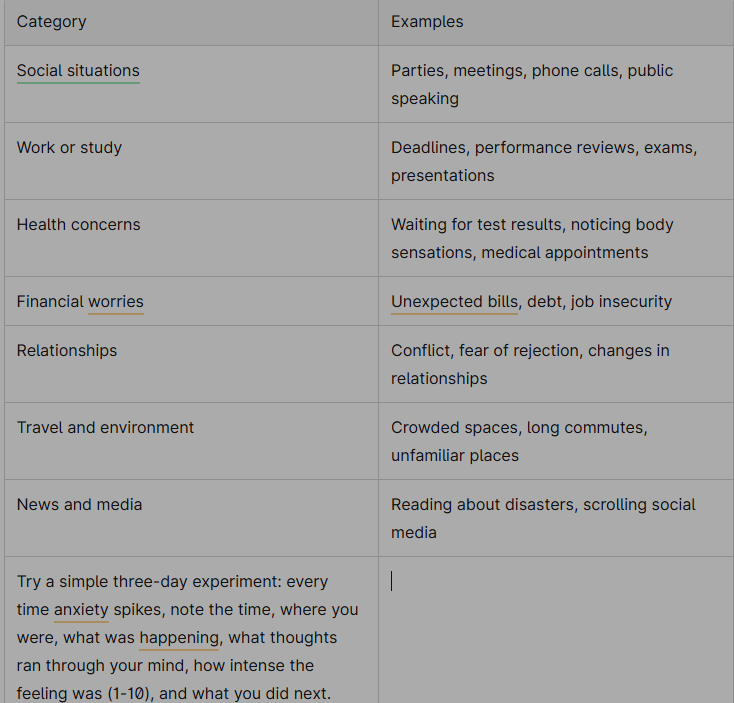
Common trigger categories include:
Try a simple three-day experiment: every time anxiety spikes, note the time, where you were, what was happening, what thoughts ran through your mind, how intense the feeling was (1-10), and what you did next. This doesn’t need to be elaborate—a few words captured in your phone is enough.
Pay attention to early warning signs that anxiety is building. For some people, it’s a clenching jaw or tight shoulders. For others, it’s a flutter in the stomach, a sudden irritability, or difficulty sitting still. Catching these early signals means you can apply coping skills before anxiety escalates.
For people living in Glasgow and other cities, specific environmental factors often serve as recurring triggers: noise, crowds, long commutes on packed trains, or the pressure of urban life. Recognising that your environment contributes to anxiety levels can help you make informed choices about when and how to manage exposure to these situations, and when to seek specialist anxiety therapy and counselling in Glasgow..
Recognising Unhelpful Thought Patterns
Anxiety doesn’t just happen to you—your thoughts play an active role in creating and maintaining it. Certain thinking styles, which cognitive behavioural therapy calls “cognitive distortions,” reliably make anxiety worse.
Catastrophising involves jumping to the worst possible outcome. “This meeting will go badly, my boss will think I’m incompetent, I’ll get fired, and I’ll never find another job.” One concern spirals into complete disaster within seconds.
Mind-reading means assuming you know what others are thinking, usually something negative about you. “Everyone at that party thought I was boring. My colleague is avoiding me because they’re angry with me.”
All-or-nothing thinking sees situations in black and white. “If this presentation isn’t perfect, it’s a complete failure.” This leaves no room for the reality that most things land somewhere in the middle.
Overgeneralising takes one instance and applies it everywhere. “I felt awkward at that dinner, so I’m terrible at social situations and always will be.”
Here’s a practical exercise: write down one anxious thought per day for a week. Then ask yourself: “What is the evidence for this thought? What is the evidence against it? What would I tell a friend who had this thought? What’s a more balanced way to see this?”
For example, if your thought is “I’ll fail this presentation,” a reframe might be: “I might feel nervous, but I can prepare thoroughly, and I’ve managed difficult presentations before. Even if it’s not perfect, it doesn’t have to be a disaster.”
This approach is a core part of cognitive behavioural therapy, which many NHS services and independent therapists offer, and structured CBT for anxiety in Glasgow often places a strong emphasis on this kind of thought challenging alongside practical exposure work. It’s not about forcing positive thinking—it’s about examining whether your automatic anxious thoughts are accurate and helpful..
Immediate Tools to Calm Anxiety in the Moment
This section gives you techniques you can use today, right now, whenever anxiety rises. Practice these when you’re only mildly stressed (perhaps on a quiet evening at home) so they become familiar and accessible when you really need them.
Breathing Exercises
4-4-8 Breathing
Breathe in slowly through your nose for 4 seconds
Hold your breath gently for 4 seconds
Exhale slowly through your mouth for 8 seconds
Repeat for 4-6 cycles (about 2-3 minutes)
The extended exhale activates your parasympathetic nervous system, signalling safety to your body. You might not feel calmer immediately, but your physiology will begin shifting.
Cyclic Sighing
Take a normal breath in through your nose
At the top of that breath, take a second, smaller sip of air
Release all the air slowly through your mouth with a sighing sound
Repeat for 2-3 minutes
Research from Stanford University found this technique particularly effective for reducing anxiety quickly, especially when paired with a calmer evening routine if you notice anxiety worsening at night..
The 5-4-3-2-1 Grounding Exercise
When anxious thoughts take over, grounding brings your attention back to the present moment and your immediate environment. This works well on a bus, in a queue, or sitting in a meeting.
5 things you can see (the texture of your sleeve, a crack in the ceiling, the colour of someone’s bag)
4 things you can touch (the chair beneath you, your feet in your shoes, the cool air on your hands)
3 things you can hear (traffic outside, the hum of air conditioning, distant voices)
2 things you can smell (coffee, your own soap or perfume)
1 thing you can taste (the lingering taste of toothpaste, tea, or just notice the inside of your mouth)
Work through each sense slowly, really noticing each thing you identify.
Progressive Muscle Relaxation (5-Minute Version)
Shoulders: Raise your shoulders up toward your ears. Hold for 5 seconds, feeling the tension. Release and notice the difference for 10 seconds.
Hands: Make tight fists with both hands. Hold for 5 seconds. Release, letting your fingers spread.
Face: Scrunch up your face—eyes closed tight, jaw clenched. Hold for 5 seconds. Release completely.
Legs: Press your feet into the floor and tense your thighs. Hold for 5 seconds. Release.
Whole body: Take a slow breath in and tense everything at once. Hold briefly. Exhale and let everything go.
The contrast between tension and release helps your body recognise what relaxation actually feels like.
How to Handle a Panic Attack Safely
When a panic attack strikes, your brain is convinced something terrible is happening. Having a plan in place helps you ride it out.
Tell yourself: “This is a panic attack. It’s uncomfortable but not dangerous. It will pass. My body is trying to protect me, even though there’s no real danger right now.”
Follow these steps:
Notice and name what’s happening. “I’m having a panic attack. My heart is racing, I feel dizzy, I can’t catch my breath. These are anxiety symptoms, not a medical emergency.”
Slow your breathing. Use the 4-4-8 technique or simply focus on making your exhale longer than your inhale. Fast breathing maintains panic; slow breathing helps settle it.
Ground yourself in your environment. Look around and describe what you see. Name five objects. Feel your feet on the floor, your back against the chair.
Use coping statements. Repeat phrases like “This will pass,” “I’ve survived this before,” “My body is safe.”
Stay in the situation if it’s safe to do so. Leaving reinforces the idea that the situation was genuinely dangerous. If you can stay (or return after the peak passes), you teach your brain that you can cope.
Ride the wave. Don’t fight the sensations. Observe them like a scientist: “My heart rate is very fast right now. It’s been about two minutes. The dizziness is still there but maybe slightly less intense.”
Positioning advice: Sit or stand with your back supported. Loosen any tight clothing around your neck or waist. Avoid rapid pacing if it worsens dizziness—slow, deliberate movement is better.
When to seek urgent help: If you experience new chest pain (especially spreading to your arm or jaw), collapse, confusion, or symptoms that feel different from your usual panic attacks, seek medical attention. It’s always better to have something checked and find it’s anxiety than to ignore a genuine medical issue.
Day-to-Day Habits That Reduce Anxiety Over Time
The techniques above help in the moment, but lasting change comes from consistent habits that lower your baseline anxiety levels over time. Small daily choices compound into significant differences, especially if you’re noticing specific patterns like anxiety before work every morning..
Sleep
Poor sleep makes anxiety worse, and anxiety makes sleep harder—a frustrating cycle. To improve both:
Keep a regular bedtime and wake time, even on weekends
Limit screens for 60 minutes before bed (the blue light and stimulating content both interfere with sleep)
Create a simple wind-down ritual: dim lights, light stretching, reading a physical book, or listening to calm music
Avoid caffeine after mid-afternoon, as it can stay in your system for hours
Getting enough sleep is one of the most effective things you can do for your mental wellbeing, and addressing patterns like evening or night-time anxiety can make restful sleep more achievable..
Physical Activity
Regular exercise rivals medication for anxiety relief in mild to moderate cases. Movement burns off the stress hormones that anxiety produces and releases endorphins that improve mood.
Aim for at least 150 minutes of moderate exercise per week (brisk walking, cycling, swimming) or 75 minutes of vigorous activity (running, intense gym classes). This might look like:
A 30-minute brisk walk five days a week
Walking along the River Clyde at lunch
Cycling to work
Dancing, yoga, or tai chi classes
A few weekly gym sessions
Even a 10-minute walk when anxiety levels are high can make a big difference. The key is consistency rather than intensity.
Food and Drink
What you consume affects how you feel:
Eat balanced meals with protein, complex carbohydrates, and vegetables to keep blood sugar and energy levels stable. Skipping meals or eating irregularly can trigger anxiety or make it worse.
Reduce caffeine, especially if you’re sensitive to it. Caffeine blocks adenosine receptors in a way that mimics the body’s arousal response—essentially giving you a chemical boost similar to anxiety.
Limit alcohol. It might feel calming initially, but it disrupts sleep and can increase anxiety the next day.
Maintain a healthy diet overall. Research suggests Mediterranean-style eating patterns correlate with lower anxiety risk.
Avoid recreational drugs, which can destabilise mood and trigger anxiety or panic attacks in susceptible people. If your anxiety leaves you feeling frozen, exhausted, or struggling to get going in the mornings, you may relate to “can’t get out of bed” anxiety and paralysis..
Regular Calm Time
Schedule time each week for activities that genuinely restore you:
Reading in a park or café
Creative hobbies (drawing, gardening, cooking, playing music)
Faith or spiritual practices if these are meaningful to you
Time with animals
Being in nature
This isn’t a luxury—it’s maintenance. Building these restorative activities into your daily routine helps manage stress before it accumulates.
Reducing Avoidance and Building Confidence
When you avoid situations that trigger anxiety, the relief feels wonderful—but it comes at a cost. Avoidance teaches your brain that the situation really was dangerous (why else would you have escaped?), which keeps anxiety strong and often makes it grow.
Exposure therapy, a core component of cognitive behavioural therapy, works by gradually facing feared situations in a controlled way. The anxiety rises at first, but if you stay in the situation long enough, it naturally decreases. Repeated exposure teaches your nervous system that the situation isn’t actually threatening, and for those with Generalised Anxiety Disorder (GAD) in Glasgow, structured support can make this process feel more manageable..
Here’s how to approach it:
Choose a fear to work on (for example, busy cafés)
Create a ladder of steps, starting with the easiest version
Rate your anxiety before and after each step (0-10)
Repeat each step until anxiety drops significantly before moving up
Celebrate small wins—each step is genuine progress
**For some people, especially those in busy cities, fears about being judged or scrutinised in public places are part of broader social anxiety difficulties in Glasgow that often respond well to targeted support.
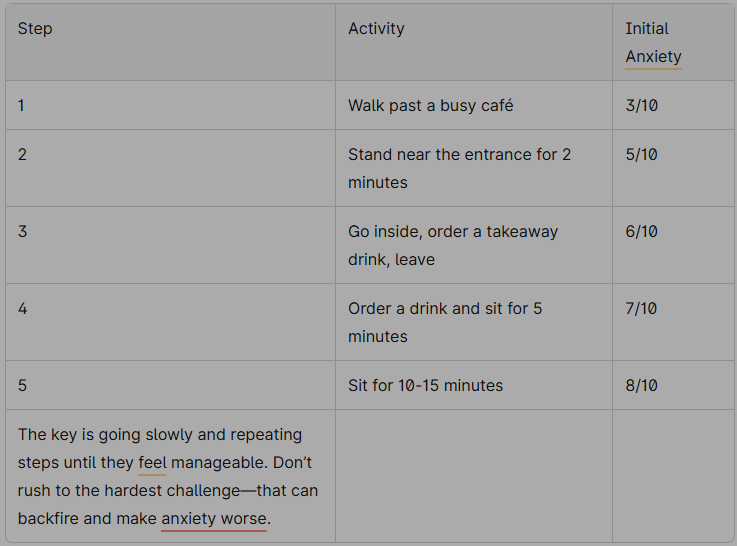
Example ladder for café anxiety::**
The key is going slowly and repeating steps until they feel manageable. Don’t rush to the hardest challenge—that can backfire and make anxiety worse.
Building Emotional Support and Professional Help
Talking about anxiety reduces shame and often halves the emotional load. Many people carry their worries in silence for years, unaware that support is available and effective, including from Glasgow anxiety specialists focused solely on anxiety treatment..
Many people now also feel more comfortable starting with online therapy for anxiety support from home, which can be especially helpful if leaving the house feels daunting.
Who to Talk To
Consider reaching out to:
A trusted friend or family member
A colleague you’re comfortable with
A community or religious leader
Peer support groups (many exist in Glasgow and other cities)
Tips for starting the conversation:
Choose a quieter time when you won’t be rushed
Be specific about what you’re experiencing (“I’ve been having these physical symptoms and constant worry”)
Say what kind of help would be useful (“I’d find it helpful if you could just listen” or “Could you come with me to my appointment?”)
If your anxiety feels urgent and is disrupting your sleep or daily functioning, you might benefit from same-day anxiety help in Glasgow alongside speaking to your usual healthcare providers.
When to See a GP or Mental Health Professional
Consider speaking to a mental health provider if:
Symptoms occur most days for several weeks
You’re experiencing panic attacks or noticing trauma-related symptoms that might benefit from EMDR or Rewind therapy for anxiety and panic
Anxiety affects your ability to work, study, or maintain relationships
You’re using alcohol or prescription drugs to cope
You’re having thoughts of self-harm
Common Treatments
A GP can discuss options and refer you appropriately. Common treatments include:
Cognitive Behavioural Therapy (CBT): The gold standard for anxiety treatment, with 50-70% sustained remission rates. Typically 8-12 weekly sessions working on thoughts and behaviours, and many people can access free NHS CBT talking therapies in the UK..
Other talking therapies: Including specialist anxiety counselling in Glasgow and psychotherapy
Group programmes: Often available through NHS services
Medication: SSRIs (like sertraline) or SNRIs (like venlafaxine) may be recommended for moderate to severe anxiety. These take 2-4 weeks to start working and are often most effective combined with therapy.
Combined approaches: Research consistently shows that psychotherapy plus medication yields better outcomes than either alone for moderate to severe cases.
Your treatment plan should be tailored to your specific situation—there’s no one-size-fits-all approach.
Online and Local Resources
Evidence-based online programmes and apps can supplement professional treatment. When evaluating these, check:
Who designed the programme (registered clinicians?)
When it was last reviewed and updated
Whether it’s based on established approaches like CBT
Many regions, including Glasgow, have community mental health organisations, peer support groups, and low-cost counselling services. NHS Scotland provides various options, including talking therapies accessible through your GP.
Make a short list of 2-3 services with phone numbers and opening hours. Keep this somewhere accessible—when anxiety is high, having the information ready makes it easier to reach out.
Remember that reaching out once is often just the beginning. It’s okay to follow up, ask questions, or try a different provider if the first option isn’t the right fit. Getting more support isn’t a failure—it’s problem-solving.
When Anxiety Is Part of Another Condition
Sometimes anxiety appears on its own; sometimes it’s intertwined with other conditions like depression, OCD, PTSD, or underlying medical conditions.
Generalised Anxiety Disorder (GAD) involves persistent, wide-ranging worry about multiple areas of life, occurring most days for at least six months and feeling difficult to control. It’s more than occasional stress about specific situations—it’s a constant background hum of “what if” thoughts that may include physical symptoms like restlessness, fatigue, and difficulty sleeping.
Obsessive-Compulsive Disorder (OCD) involves intrusive, unwanted thoughts (obsessions) that cause anxiety, and repetitive behaviours or mental acts (compulsions) performed to relieve that anxiety. This might look like repeated checking, cleaning, counting, or seeking reassurance. OCD often requires specialist therapy for OCD and intrusive thoughts beyond standard anxiety treatment..
Post-Traumatic Stress Disorder (PTSD) can develop after traumatic past experiences and includes symptoms like flashbacks, nightmares, intense emotional reactions to reminders of the trauma, and avoidance of related situations. Trauma-focused therapies like EMDR or trauma-focused CBT are typically recommended.
Depression commonly occurs alongside anxiety. The depression association with anxiety means if you’re experiencing persistent low mood, loss of interest in activities, and feelings of worthlessness alongside anxiety, it’s worth mentioning both to a professional, and exploring options such as self-referral to NHS mental health services where available..
Avoid self-diagnosing based solely on online information. Instead, use what you notice about your symptoms as a starting point for conversation with a GP or therapist who can assess properly and recommend appropriate help.
FAQ
Can Anxiety Cause Real Physical Health Problems?
Anxiety itself isn’t usually dangerous, but chronic high stress can contribute to other symptoms like tension headaches, muscle pain, digestive issues, and elevated blood pressure over time. The body wasn’t designed to stay in fight-or-flight mode constantly.
Any new or worrying physical symptom should still be checked by a GP rather than assuming it’s “just anxiety.” Many conditions share symptoms with anxiety, and ruling out medical causes is important for both your peace of mind and your health; once serious issues are excluded, resources on anxiety-related chest symptoms rather than heart problems can be reassuring..
The good news: learning to manage stress and anxiety typically improves both mental and physical wellbeing. Techniques that ease anxiety also help your body recover from chronic stress.
Is It Possible to Completely Get Rid of Anxiety?
The goal isn’t to eliminate anxiety entirely—that wouldn’t be possible or even desirable. Anxiety is a normal human emotion that sometimes protects us and motivates us. The aim is to reduce how intense anxiety feels, how often it appears, and how much it interferes with your personal life.
Most people can significantly reduce their anxiety through a combination of self-help strategies, lifestyle changes, and professional support when needed. Many find they can live full, active lives even if some anxiety remains, including those dealing with social anxiety who access targeted therapy in Glasgow..
Focus on “living well with anxiety” rather than waiting until all anxious feelings disappear before engaging in valued activities. You can cope with anxiety while building the life you want.
How Can I Help a Partner, Friend, or Family Member With Anxiety?
Start by listening without immediately trying to fix things. Validate their feelings (“That sounds really difficult”) rather than dismissing them (“You’ll be fine, don’t worry about it”). Ask what kind of support they find most helpful—some people want advice, others just want someone to listen.
Practical help can include:
Offering to accompany them to appointments
Practising breathing exercises or grounding together
Helping break overwhelming tasks into small targets
Being patient with avoidance behaviours while gently encouraging progress
Look after your own wellbeing too. Supporting someone with anxiety can be draining, and it’s important to maintain your own boundaries. If you feel overwhelmed or unsure how to help, it’s okay to seek guidance yourself.
Can Lifestyle Changes Really Make a Difference If My Anxiety Feels Severe?
When anxiety is intense, suggestions like “go for a walk” or “eat well” can sound dismissive. However, research shows that lifestyle changes do help—not as a replacement for professional treatment, but as part of a comprehensive approach that improves resilience and treatment outcomes.
If your anxiety feels severe, seek professional help first. Then, start incorporating lifestyle changes gradually—one consistent change at a time rather than trying to overhaul everything at once. A 10-minute daily walk or a regular sleep schedule is a realistic starting point.
Think of lifestyle changes as building a foundation. They work best alongside, not instead of, professional treatments for moderate to severe anxiety.
What If I Feel Worse When I First Start Facing My Fears?
This is completely normal and expected. When you face something you’ve been avoiding, anxiety rises at first because you’re doing something new and challenging. Your brain is still operating under the old belief that this situation is dangerous.
The key is going slowly, repeating steps until anxiety drops, and using coping skills along the way. With repeated exposure, anxiety typically decreases and confidence grows. Most people find that what felt unbearable initially becomes manageable with practice.
If exposure feels overwhelming or you’re unsure how to design a safe plan, work with a therapist who specialises in anxiety. They can help you create a graduated approach and provide support through the process. Feeling worse temporarily doesn’t mean the approach isn’t working—it often means you’re on the right track.