Therapists for Health Anxiety: How to Find the Right Support and What to Expect
Key Takeaways
Health anxiety (also called illness anxiety disorder) is highly treatable, with cognitive behavioural therapy (CBT) recommended as the primary approach by NICE guidelines in England and Wales.
You can access therapists for health anxiety through NHS Talking Therapies, private clinics, or online—with options available across the UK including London, Manchester, Birmingham, and beyond.
Look for therapists with accredited qualifications (BABCP, BACP, or HCPC registration), specific experience with health anxiety or OCD, and someone you feel comfortable working with.
Therapy typically combines education about how anxiety works, structured work on thoughts and behaviours, and practical tools to reduce checking and reassurance seeking.
Many people experiencing health anxiety see noticeable improvement within 8–20 sessions, though progress is gradual and tailored to individual needs.
What Is Health Anxiety and When Should You See a Therapist?
Health anxiety is a persistent, excessive worry about having or developing a serious illness—despite medical reassurance and negative test results. If you find yourself constantly worrying about symptoms like headaches, chest tightness, or skin changes, convinced they signal cancer, a heart attack, or another severe illness, you may be dealing with this condition.
The terminology around health anxiety can be confusing. Historically, it was called hypochondria, but modern diagnostic manuals use different terms. Illness anxiety disorder refers to persistent health fears without prominent physical symptoms, while somatic symptom disorder applies when someone experiences physical symptoms alongside excessive health worries. Cyberchondria—the compulsive need to search symptoms online—has become increasingly common in the digital age. These labels overlap, but what matters most is recognising the pattern: you fear serious medical conditions despite evidence suggesting you’re okay.
Typical health worries include:
Repeatedly checking moles for signs of melanoma
Monitoring your heartbeat for irregularities that might indicate a heart attack
Obsessing over headaches as possible brain tumours
Interpreting muscle tension or fatigue as symptoms of neurological disease
Noticing body sensations that others would ignore and catastrophising their meaning
It’s important to understand that health anxiety can coexist with genuine health conditions. Someone with diabetes or IBS can still develop excessive, disproportionate fear about their own health. Therapy focuses on the anxiety patterns—the constant checking, the catastrophic thinking, the inability to accept medical reassurance—rather than dismissing real health needs.
When to Seek a Therapist
Consider reaching out for professional support if you recognise these signs:
Your anxiety about illness has lasted six months or longer
You spend significant time daily checking your body, Googling symptoms, or seeking reassurance
You avoid normal activities like exercise, travel, or socialising because of health fears
Frequent GP visits or medical tests provide little lasting relief
Your worry about your own health is affecting work, relationships, or quality of life
A close relative or family member has expressed concern about your preoccupation with illness
Common Signs and Symptoms Therapists Look For
When you meet with health anxiety therapists, they assess both the thoughts running through your mind and the behaviours you’ve developed around health concerns. This isn’t just about physical sensations—it’s about understanding the full picture of how health worries have shaped your daily life.
Mental Symptoms
Constant fear of having or developing a serious health condition
Catastrophic thinking patterns (“this headache must be a stroke,” “this mole is definitely cancer”)
Inability to accept medical reassurance, even after normal test results
Intrusive thoughts about hospitals, dying, or leaving loved ones behind
Difficulty concentrating on anything other than potential symptoms
A person believes that doctors have missed something despite thorough examinations
Behavioural Patterns
Repeated body checking (monitoring pulse dozens of times daily, examining skin in mirrors)
Excessive symptom Googling and reading medical forums
Seeking reassurance from doctors, partners, or friends multiple times per week
Avoiding medical TV programmes, health news, or conversations about illness
Either frequently visiting doctors or avoiding them entirely out of fear of bad news
Requesting repeated medical tests for the same concern
Physical Symptoms Driven by Anxiety
Here’s where things get complicated. Anxiety itself produces physical sensations that can feel terrifyingly real:
Racing heart and palpitations
Dizziness and lightheadedness
Nausea and digestive upset
Muscle tension and aches
Chest tightness and shortness of breath
Tingling sensations in hands or face
Panic attacks with overwhelming physical intensity
These symptoms are generated by your nervous system responding to perceived threat. But when you’re already worried about your health, experiencing a racing heart can feel like confirmation of the heart disease you fear—creating a vicious cycle.
People with health anxiety often notice that anxiety about a symptom actually makes the symptom worse, which then increases the anxiety further.
Overlap with OCD
Therapists also look for patterns that resemble obsessive compulsive disorder: obsessional health fears paired with compulsive checking and reassurance seeking. The difference can be subtle, and many people experience elements of both. A skilled health anxiety specialist can help distinguish between these presentations and ensure treatment addresses your specific needs.
Why Work with a Therapist for Health Anxiety?
If you’ve tried to manage health anxiety on your own—perhaps by telling yourself to stop Googling, or trying to ignore symptoms—you’ve likely discovered how difficult this is. Self help alone often isn’t enough because health anxiety operates in a self-reinforcing cycle.
The pattern typically looks like this: you notice a body sensation, fear kicks in, you check or seek reassurance, you feel temporary relief, doubt creeps back in, and the cycle repeats. Each round of reassurance seeking actually strengthens the anxiety over time, teaching your brain that the threat was real and that checking was necessary.
Therapists provide structured support to break this cycle. They help you identify your specific triggers, challenge the unhelpful thoughts driving your fear, and gradually reduce anxiety without relying on checking behaviours or medical reassurance.
What the Evidence Says
NICE (National Institute for Health and Care Excellence) recommends psychological therapies, particularly cognitive behavioural therapy, as the first-line treatment for health anxiety and related conditions in England and Wales. Research shows that CBT achieves response rates of 50–70%, with many patients maintaining improvements at six-month follow-up.
Benefits Reported by People Who Complete Therapy
Fewer emergency GP or A&E visits driven by panic rather than genuine need
More confidence doing normal activities like using public transport, going to the gym, or travelling
Less time spent preoccupied with bodily sensations and checking behaviours
Improved ability to tolerate uncertainty about health without spiralling
Better relationships, as loved ones are no longer constantly asked for reassurance
Return to a more normal life with space for work, hobbies, and family
Therapists can also coordinate with your GP or a psychiatrist if medication (such as SSRIs) is considered as additional support. This integrated approach often produces the best clinical outcomes for people with more severe or longstanding health anxiety.
Types of Therapy Used by Health Anxiety Specialists
No single therapy suits everyone. The right approach depends on your specific patterns, preferences, and whether past experiences like trauma play a role in your health fears. Many therapists integrate more than one method—for example, combining CBT with mindfulness techniques.
What matters is finding an approach that fits your needs and a therapist who can deliver it skilfully.
Cognitive Behavioural Therapy (CBT) for Health Anxiety
NICE recommends cognitive behavioural therapy CBT as the primary treatment for health anxiety and illness anxiety disorder. It’s the most extensively researched approach, with strong evidence supporting its effectiveness.
CBT works by helping you understand the connections between thoughts, feelings, and behaviours. In health anxiety treatment, this means:
Identifying catastrophic thoughts: Learning to notice when you’re jumping to worst-case conclusions (“this pain must be cancer”)
Questioning the evidence: Examining whether your fears match reality (“what’s the actual probability?”)
Behavioural experiments: Testing predictions by delaying checking and observing what happens
Graded exposure: Gradually facing feared situations, like exercising without monitoring your heart rate
Response prevention: Reducing compulsive checking and reassurance seeking
A typical course of CBT involves weekly 50–60 minute sessions for around 8–20 weeks, with structured homework exercises between sessions. You’ll likely keep diaries, practise new responses to anxiety, and gradually start resuming activities you’ve been avoiding.
CBT can be delivered face to face at clinics in London, Birmingham, Manchester, and other UK cities, or via secure video sessions across the country. This approach suits people who appreciate practical strategies, worksheets, and clear action plans.
Acceptance and Commitment Therapy (ACT) and Mindfulness-Based Approaches
ACT is a modern, evidence based therapy that takes a different angle. Rather than trying to eliminate anxious thoughts, ACT focuses on changing your relationship with them.
For health anxiety, ACT includes:
Mindfulness exercises to notice physical sensations without immediately reacting
“Defusion” techniques—learning to see thoughts like “I have cancer” as mental chatter rather than facts
Clarifying personal values (like spending time with family or pursuing career goals) to guide behaviour instead of fear
Practising acceptance of uncertainty rather than fighting it
Mindfulness based cognitive therapy (MBCT) is often integrated into treatment, typically delivered in an 8-week group format. Participants learn practices like body scans—observing sensations without judgement—alongside education about how avoidance amplifies health worries.
These approaches suit people who struggle with uncertainty and perfectionism, and who are open to reflective or meditative exercises. They can be particularly helpful for preventing relapse in chronic cases.
EMDR and Trauma-Focused Therapies
Eye movement desensitisation and reprocessing (EMDR) was originally developed for trauma, but it’s increasingly used when health anxiety is linked to past experiences—perhaps an intensive care stay, cancer treatment, a serious childhood illness, or witnessing ill health in a family member.
EMDR helps reprocess distressing memories (like frightening hospital experiences) that continue to fuel panic about new symptoms. The therapy involves recalling the traumatic memory while engaging in bilateral stimulation (typically guided eye movements), which appears to help the brain process the memory differently.
Some UK clinics offer EMDR combined with CBT specifically for health anxiety, both face-to-face and online. This approach is particularly relevant if your anxiety began after a clear medical event or after a close relative experienced severe illness. If you are experiencing social anxiety, specialized therapy and counselling options are also available.
Person-Centred, Integrative, and Holistic Therapies
Person-centred therapy takes a client-led, non-directive approach. The therapist offers empathy and a safe space to explore your fears around illness, death, and vulnerability without pushing specific techniques.
Integrative therapists may combine CBT techniques with relational and body-focused work, helping you feel safer in your body rather than constantly monitoring it for danger. Some clinics include creative arts therapies, relaxation techniques, and family work alongside individual sessions.
These therapy options suit people who want to explore deeper emotional themes—perhaps how past experiences, attachment patterns, or unresolved grief contribute to current health fears—rather than focusing solely on checking behaviours.
How to Find a Therapist for Health Anxiety in the UK
You can access therapy through the NHS, charities, or private clinics. Each route has different waiting times, costs, and formats. Many people find that understanding all their options helps them make the best decision for their situation.
NHS Routes
Speak to your GP: They can refer you to local mental health services and rule out any medical conditions first
Self referral to NHS Talking Therapies: In England, you can refer yourself directly to local psychological therapies services (formerly called IAPT) without seeing your GP first
Ask specifically about health anxiety: When self-referring, mention that you’re experiencing health anxiety or illness anxiety disorder, as some services have practitioners with relevant expertise
Be prepared for waiting times: NHS services are free but waiting lists can be several months in some areas
Finding Private Therapists
Practical Considerations
Many private therapists offer online video sessions across the UK, not just in major cities
Initial phone consultations (often 15–20 minutes, sometimes free) let you discuss fit before committing
Typical private fees range from £50–£120 per 50-minute session, varying by location and therapist experience
Some training clinics and charities offer lower-cost therapy options with supervised trainees
Ask about cancellation policies and whether sessions can be rescheduled
Many people find it helpful to contact 2–3 therapists before deciding. A brief conversation can tell you a lot about whether you’ll feel comfortable working together.
Choosing the Right Health Anxiety Specialist
The relationship with your therapist matters as much as their techniques. Feeling safe, understood, and not judged is foundational to effective therapy. Research consistently shows that therapeutic alliance—the connection between you and your therapist—predicts outcomes across different therapy types.
Qualifications to Look For in the UK
Questions to Ask Prospective Therapists
What experience do you have working with health anxiety and OCD-style checking?
What’s your typical approach to treating health anxiety?
How long does treatment usually take, and how is it structured?
Do you offer CBT, ACT, EMDR, or other specific modalities?
How do you handle situations where I’m seeking medical reassurance in sessions?
Can you work with my GP if needed?
Practical Checkpoints
Appointment availability (evenings, weekends?)
Online vs in-person options
Clinic location and accessibility
Cancellation and rescheduling policies
Fee structure and payment timing
Whether they provide between-session support
Trust Your Instincts
After an initial consultation, notice how you feel. Did the therapist seem to understand health anxiety specifically? Did they balance empathy with clear guidance? Did you feel believed about your distress? A good fit means you can be honest about your fears without feeling dismissed or judged.
What to Expect in Therapy for Health Anxiety
Starting therapy can feel daunting, especially when you’re already anxious. It helps to know that early sessions focus on understanding your story rather than forcing immediate change.
Your First Session
A typical first session involves:
Discussing your current health worries and how they affect daily life
Reviewing relevant medical history and past experiences with doctors
Understanding how often you seek reassurance, check symptoms, or visit the GP
Exploring when the anxiety started and any triggers (like a serious childhood illness or a family member’s ill health)
Discussing what you hope to achieve—perhaps fewer panic-driven A&E visits, ability to travel without fear, or simply reclaiming your normal life
Assessment
Your therapist may use structured questionnaires (like the Health Anxiety Inventory) alongside conversation to map severity and patterns. This isn’t about labelling you—it’s about understanding exactly how health anxiety shows up in your life so treatment can be tailored accordingly.
Your Treatment Plan
Together, you’ll agree on:
Specific goals (reducing Google searches, practising response prevention, addressing fear of death)
Which strategies to prioritise
Expected number of sessions
How you’ll measure progress
This collaborative approach means you’re an active participant, not a passive recipient.
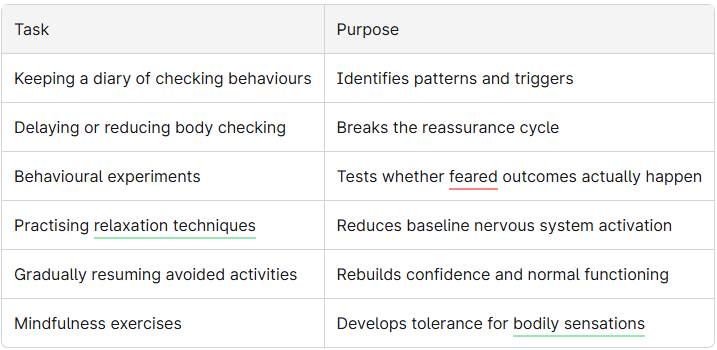
Common Therapy Tasks
Progress Takes Time
Improvement is often gradual and non-linear. You might have good weeks followed by harder ones, especially when stress increases. Therapists regularly review what’s helping and adapt the plan. The goal is stable, lasting change over months rather than quick fixes that don’t hold.
Self-Help Strategies While You Look for a Therapist
Waiting lists and costs mean many people start with self help while arranging formal therapy. These strategies won’t replace professional support for severe health anxiety, but they can stabilise day-to-day life and make therapy more effective when it begins.
Keep a Simple Daily Log
Track triggers, thoughts, checking behaviours, and how long anxiety episodes last. This record becomes valuable when you start therapy—your therapist can see patterns you might not notice yourself.
Create Worry Windows
Designate 10–15 minutes once or twice daily as your “worry time.” When health fears arise outside these windows, briefly note them and postpone engaging until your scheduled time. This begins reclaiming attention for other activities.
Reduce Symptom Googling
Choose one trusted medical information source (like NHS.uk) rather than multiple forums
Set a daily time limit for health searches
Consider having a family member change your browser settings to block health forums temporarily
Notice the temporary relief versus the longer-term anxiety increase that Googling produces
Alternative Responses to Anxiety Spikes
Instead of checking or seeking reassurance:
Go for a short walk
Phone a friend about something unrelated to health
Shift focus to a valued activity (reading with children, cooking, gardening)
Practise a brief breathing exercise (slow exhale longer than inhale)
Use relaxation techniques like progressive muscle tension release
Coping Mechanisms to Reduce Anxiety
Maintain regular sleep patterns
Limit caffeine and alcohol, which can amplify physical sensations
Exercise regularly (this actually reduces generalised anxiety and muscle tension)
Stay connected with friends and activities that matter to you
Consider apps offering guided mindfulness for anxiety
Self-help can make a real difference, but if your health anxiety is severe—causing panic attacks, significant avoidance, or mental health problems affecting work and relationships—professional support is the recommended treatment.
FAQ: Therapists for Health Anxiety
How long does therapy for health anxiety usually take?
If you have found that anxiety medication isn't working for you, many people notice meaningful improvement after 8–12 CBT sessions. However, more longstanding or complex cases—especially those involving trauma, multiple mental health problems, or middle age onset after decades of worry—may benefit from 20+ sessions. Some people find periodic “top-up” appointments over a year help maintain gains and manage health worries during stressful periods.
Can I have therapy for health anxiety if I also have a medical diagnosis?
Absolutely. Therapists regularly work with people who have chronic conditions like diabetes, IBS, or heart disease. Treatment focuses on reducing excessive worry and compulsive checking while respecting necessary medical care. Having a genuine health condition doesn’t mean your anxiety about it is proportionate—therapy helps you manage health anxiety without ignoring legitimate medical needs.
Is online therapy as effective as in-person sessions for health anxiety?
Research suggests video-based CBT and related evidence based therapies can be as effective as face-to-face for many anxiety disorders, including health anxiety. The key factors are structured sessions, confidentiality, and a good therapeutic relationship. Online therapy expands access for people outside major cities or with mobility limitations. Some people prefer the convenience; others feel they connect better in person. Many therapists offer both options.
Will a therapist tell me my symptoms are “all in my head”?
Ethical therapists do not dismiss physical symptoms. They encourage appropriate medical checks when needed and will never tell you to ignore genuine health concerns. What they will help you notice is when anxiety—rather than actual illness—is driving ongoing fear, excessive worry, and checking. The aim is to help you respond to symptoms proportionately, not to deny your experience.
What if I’m afraid therapy will make me focus even more on my symptoms?
This is a common concern. While therapy does involve talking about your fears initially, sessions are designed to give you tools and new perspectives. Over time, most people find they spend less of their day focused on symptoms and more on work, relationships, and activities that bring meaning. Therapists are trained to pace treatment so you feel supported rather than overwhelmed. If something isn’t working, a good therapist will adjust the approach.